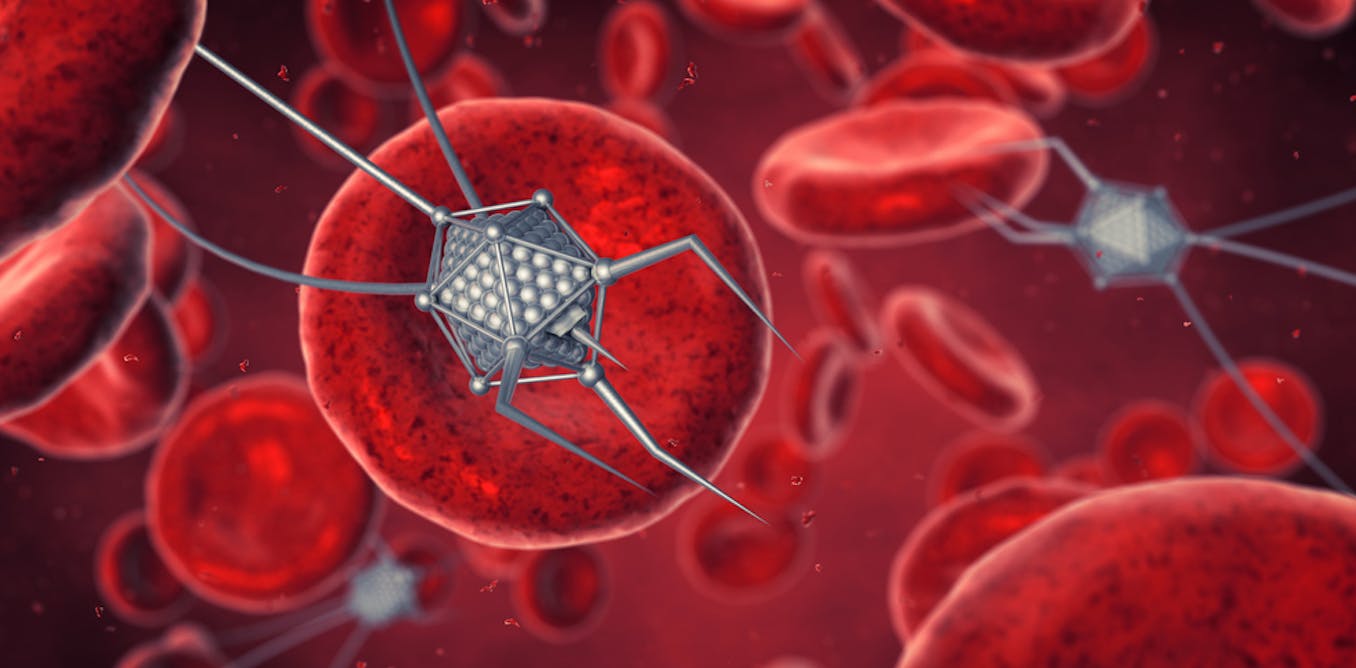
Ever wondered how tiny particles revolutionized medicine? Dive into the captivating. history of nanomedicine. Explore how these minuscule wonders have transformed healthcare practices worldwide. From targeted drug delivery to advanced imaging techniques, nanomedicine has opened new frontiers in medical treatment. Ready to unravel the mysteries behind this groundbreaking field?
Evolution of Nanomedicine
Conceptual Origins
Nanomedicine, a field focusing on manipulating matter at the nanoscale, was first proposed by physicist Richard Feynman in 1959. The essence of nanomedicine lies in exploring new healthcare possibilities through nanotechnology. This concept emerged from the desire to revolutionize medical treatments using tiny particles.
Historical Development
Advancements in nanotechnology gained momentum in the 1980s, leading to significant breakthroughs in nanomedicine during the late 1990s and early 2000s. The historical progress of this field has been fueled by collaborations between scientists, engineers, and medical professionals. These interdisciplinary efforts have propelled nanomedicine into an innovative domain within healthcare.
Pioneers in Nanotechnology
Key figures like Richard Feynman, Eric Drexler, and Norio Taniguchi are pioneers in advancing nanotechnology. Feynman’s groundbreaking lecture laid down the fundamentals for exploring matter at an atomic level. Drexler’s book popularized the notion of nanotechnology and its vast applications across various industries.
Initial Commercial Applications
The initial commercial uses of nanomedicine centered around drug delivery systems and diagnostic tools. Nanoparticles played a crucial role in enhancing drug solubility and refining targeted drug delivery techniques. Moreover, nanoparticle-based imaging agents transformed conventional medical imaging practices.
Nanoscience and Technology in Medicine
Nanomedicine is all about using nanotechnology in medicine. It focuses on diagnosis, treatment, and disease prevention by designing materials at the nanoscale to interact with biological systems. This field offers solutions for personalized medicine and targeted therapies.
For example, scientists can create tiny particles that carry drugs directly to cancer cells without harming healthy tissues. These nanoparticles are so small they can pass through barriers in the body that traditional medicines cannot.
Importance in Human Health
Nanomedicine has the potential to transform healthcare by providing precise diagnostics and targeted treatments. It allows early detection of diseases, enhances drug delivery methods, and improves imaging technologies. By making treatments more effective and efficient, it helps reduce side effects for patients.
Imagine a scenario where doctors can use tiny sensors made from nanomaterials to detect diseases like Alzheimer’s much earlier than current methods allow. This could lead to better outcomes for patients as treatment could start sooner when it is most effective.
Government and Corporate Support
Funding Initiatives
Governments, private organizations, and research institutions play a crucial role in advancing nanomedicine through funding initiatives. These programs aim to speed up the transition of nanomedicine from the lab to real-world medical applications. By supporting interdisciplinary collaboration, these funding schemes drive innovation in nanomedicine. For instance:
- The National Institutes of Health (NIH) in the U.S. offers grants for nanotechnology-based medical research.
- The European Commission provides funding through programs like Horizon 2020 for nanomedicine projects.
Collaborative efforts between various stakeholders ensure that promising nanomedical discoveries are translated into practical solutions for healthcare challenges.
Regulatory bodies enforce strict requirements for the approval and commercialization of nanomedicines, ensuring their safety and efficacy before reaching patients. These agencies meticulously evaluate every aspect of nanomedicines, including manufacturing processes and labeling practices, to safeguard public health. Guidelines specifically tailored for characterizing and producing nanomedical products have been established to maintain quality standards across the industry.
- The Food and Drug Administration (FDA) in the U.S. oversees regulatory approvals for nanotechnology-based drugs.
- The European Medicines Agency (EMA) sets stringent criteria for assessing the quality and performance of nanoscale medicines.
Public Awareness and Controversy
Media plays a significant role in how people perceive nanomedicine. News articles, TV shows, and social media can influence what the public thinks about the benefits and risks of using nanotechnology in medicine. Responsible reporting by the media is crucial to ensure that accurate information is shared with the public.
Ethical issues are important. Privacy concerns, making sure patients understand their treatment, ensuring fair access to treatments for everyone, and considering any unintended consequences are all part of these ethical considerations. It’s challenging to balance individual rights with what’s best for society in this field.
Developing ethical guidelines is essential as nanomedicine evolves. These frameworks will help address new ethical dilemmas that may arise as technology advances. By setting clear rules on privacy, consent, fairness, and potential risks early on, we can navigate the complexities of integrating nanotechnology into healthcare more smoothly.
Clinical Aspects of Nanomedicine
Lipid-based Nanomedicines
Lipid-based nanomedicines use lipid nanoparticles to deliver drugs, enhancing solubility and stability. These nanoparticles can target specific tissues and cells effectively. For instance, lipid carriers encapsulate hydrophobic drugs for better delivery.
One advantage is the ability to improve drug effectiveness while reducing side effects. However, challenges include potential toxicity concerns with certain lipid formulations.
- Pros: Enhanced drug solubility and targeted delivery.
- Cons: Toxicity issues with specific lipids.
Antimicrobial Nanomedicine
Antimicrobial nanomedicine employs nanoparticles to combat infections by disrupting microbial membranes or inhibiting growth. This approach offers promising solutions against antibiotic resistance and infectious diseases. By improving antibiotic efficacy, these nanoparticles play a crucial role in fighting infections efficiently.
The use of antimicrobial nanomedicine can help address the growing concern of antibiotic-resistant bacteria worldwide.
- Key Information: Enhances antibiotics’ effectiveness against resistant strains.
Advancements in Drug Delivery
Nanoparticle-based Systems
Nanoparticle-based systems are like tiny delivery vehicles for drugs, imaging agents, and therapies. Scientists can precisely design these systems by controlling their size, shape, and surface properties. For example, they can load specific amounts of drugs onto nanoparticles to target them to the right places in the body.
These drug delivery systems have shown great potential in targeted therapy and molecular imaging. They work like guided missiles that deliver treatments directly to where they are needed most. This precision helps reduce side effects and improve treatment outcomes significantly.
Targeting Peptides
Targeting peptides act as GPS signals for nanomedicines, guiding them to specific cells or tissues in the body. These short amino acid sequences bind specifically to receptors on target cells, ensuring that the medicine reaches its intended destination accurately. By using targeting peptides with nanomedicines, scientists can enhance their effectiveness while minimizing unintended effects outside the target area.
- Pros:
- Enhanced drug efficacy
- Reduced off-target effects
Future Prospects in Nanomedicine
Next Generation Nanomedicines
Next-generation nanomedicines are the future of healthcare. They use cutting-edge materials and technology to improve treatment effectiveness while reducing side effects. Imagine tiny robots delivering medicine precisely where it’s needed in your body, like a targeted missile aiming for a specific spot. These advanced medicines are like personalized superheroes fighting diseases inside you.
The development of next-generation nanomedicines involves high-tech tools such as gene editing, which is like having a microscopic surgeon fixing genetic issues at the molecular level. These futuristic treatments could revolutionize how we combat diseases by making therapies more efficient and less harmful to our bodies.
Nanosimilars Development
Nanosimilars are generic versions of advanced medicines that mimic the original drug’s quality and safety standards. Think of them as identical twins to expensive branded medications but more affordable. The creation of nanosimilars requires detailed testing to ensure they work just as well as their pricier counterparts without compromising on safety or efficacy levels.
These cost-effective alternatives make sophisticated treatments accessible to more people who need them, expanding healthcare options globally and improving overall patient care.
Summary
You’ve journeyed through the evolution of nanomedicine, exploring its impact on healthcare. From the intersection of nanoscience and medicine to the support from governments and corporations, you’ve seen how nanomedicine is shaping the future of healthcare. Despite public awareness and some controversies, the clinical applications and advancements in drug delivery are paving the way for a new era in medicine. The future holds exciting prospects for nanomedicine, promising innovative treatments and personalized care that could revolutionize how we approach health and wellness.
As you reflect on the strides made in nanomedicine, consider how this field could transform healthcare in the years to come. Stay curious, stay informed, and be part of the conversation driving these groundbreaking changes. Embrace the possibilities that nanomedicine offers and envision a future where precision medicine is not just a concept but a reality. Keep exploring, keep learning, and be ready to embrace the future of healthcare with open arms.
Frequently Asked Questions
What is the significance of the evolution of nanomedicine?
The evolution of nanomedicine represents a groundbreaking shift in healthcare, merging nanotechnology with medicine to enhance treatment precision and effectiveness. It opens doors to innovative therapies that target diseases at a cellular level, promising improved patient outcomes and reduced side effects.
How does nanoscience contribute to advancements in medicine?
Nanoscience enables the development of tiny particles that can deliver drugs directly to targeted cells, improving drug efficacy while minimizing side effects on healthy tissues. By harnessing nanoparticles’ unique properties, researchers are revolutionizing drug delivery systems for more personalized treatments.
Why is public awareness crucial in understanding nanomedicine?
Public awareness plays a pivotal role in fostering trust and acceptance of nanomedicine innovations. Educating the public about its benefits helps dispel misconceptions and encourages support for further research and development. Increased awareness also promotes informed decision-making among patients regarding novel treatment options.
What are some key clinical aspects associated with nanomedicine applications?
Clinical aspects of nanomedicine encompass rigorous testing for safety and efficacy before widespread adoption. Researchers focus on determining optimal dosages, potential side effects, and long-term impacts on patient health. Clinical trials play a vital role in validating the effectiveness of nano-based therapies across various medical conditions.
How do advancements in drug delivery through nanotechnology benefit patients?
Advancements in drug delivery using nano-sized carriers offer precise targeting of diseased cells, enhancing therapeutic outcomes while reducing systemic toxicity. This approach allows for lower medication doses with higher efficiency, leading to fewer adverse reactions and improved quality of life for patients undergoing treatment.